IASLC World Conference on Lung Cancer
allautoe 0 GECP congresses news
Hereditary predisposition plays a larger role in SCLC development than previously recognized and may inform personalized treatment
Dr Nobuyuki Takahashi, from the Center for Cancer Research (CCR) of the National Cancer Institute (NCI) in Bethesda, Maryland, presented at the “2020 IASLC World Conference on Lung Cancer” (which took place between 27 and 31 January 2021) a work that reveals important conclusions: Complete exome sequencing shows that almost half of patients with small cell lung cancer (CPPC) have a germline mutation that may be associated with the development of the disease, and these mutations could lend for targeted therapy and screening in about 10% of individuals.
Dr. Takahashi and colleagues performed whole-exome sequencing of germline DNA from peripheral blood mononuclear cells taken from 77 individuals with SCLC and 10 individuals with extrapulmonary small cell cancer. This discovery cohort consisted of individuals recruited across the United States for participation in NCI-sponsored clinical trials, all of whom had previously received platinum-based chemotherapy.
After sifting through 607 genes associated with the development of cancer, the researchers found that 43.7% of patients within the cohort harbored a pathogenic or likely pathogenic mutation in 35 genes. In 9 patients (10.3%) the genetic variants identified were deemed to be actionable, offering up the opportunity for genetic counseling and screening for the patients and their family members.
Notably, two-thirds of the germline mutations identified occurred within genes involved in DNA damage repair pathways. Whole-exome sequencing revealed loss of heterozygosity of MLH1, BRCA2, and SMARCA4, emphasizing the importance of these genes in tumor formation and as potential treatment targets.
When Dr. Takahashi’s group applied the same germline whole-exome sequencing process to an independent cohort of 79 patients with SCLC, they found that a similar proportion of individuals—40.2%—harbored a deleterious germline mutation, validating their initial results. Moreover, the types of mutations were also similar, with genes involved in DNA damage repair again predominating.
In another validation step, the group compared the sequencing results for the NCI cohort with those from a cohort of more than 53,000 cancer-free individuals from the Exome Aggregation Consortium (ExAC). Germline mutations within MUTYH, CHEK1, RAD51D, and BRCA2 were roughly 6 to 4,000 times more likely to be found in the NCI cohort with SCLC as compared with the cancer-free ExAC cohort.
In evaluating whether the pathogenic mutations were linked to clinical characteristics, the investigators found that germline genotype correlated with a higher likelihood of having a first-degree relative with a history of cancer (odds ratio [OR] 1.82) or lung cancer (OR 2.60).
Individuals with a germline genotype showed a 56% reduction in the risk of recurrence (HR 0.44) following platinum-based chemotherapy as compared with individuals lacking such mutations.
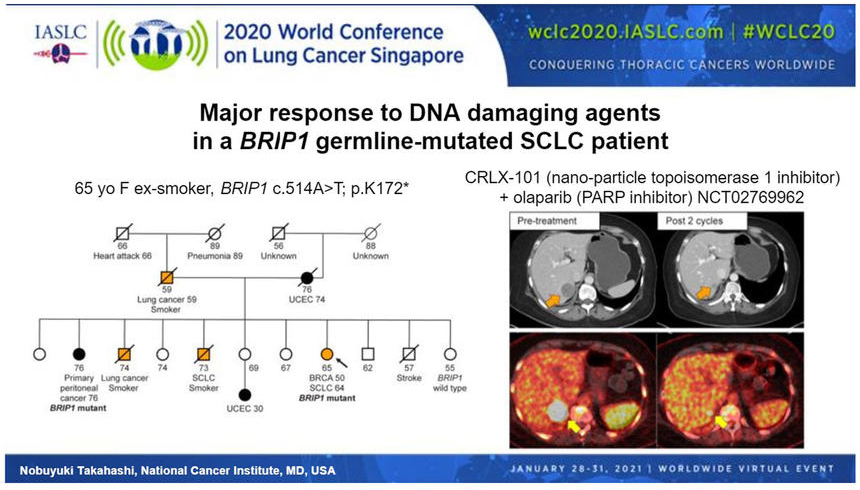
The relevance of these observations for therapeutics was tested in a single patient with SCLC and a germline BRIP1 mutation. BRIP1 is involved in the BRCA1 complex, and its monoallelic pathogenic germline mutation is associated with a high risk of ovarian cancers. Indeed, the patient had multiple family members with endometrial cancer or lung cancer, and her sister had primary peritoneal cancer harboring the same BRIP1 variant (Figure). Treatment of the patient with a topoisomerase 1 inhibitor, in combination with a PARP inhibitor, resulted in a 64% reduction in the size of the patient’s liver lesion and resolution of pain.
Overall, these findings suggest that SCLC may have an inherited predisposition, and this could have substantial implications for targeted therapy and directed cancer screening forSCLC patients and their families.
